
The more complete and competent the diagnosis of prostatitis, the more effective the subsequent treatment will be. A formal doctor approach can lead to long-term and ineffective treatment for the patient. Its purpose is to identify inflammation of the prostate and all the factors that cause it.
How Doctors Diagnose Prostatitis
Receive anonymity
During the initial consultation, the doctor will ask the following questions:
- Duration of sexual intercourse (if it became shorter, then under what conditions)?
- The presence of inguinal discomfort during prolonged stay in a static position, as well as after alcohol consumption or hypothermia. Frequency and speed of urination (there are difficulties, intermittent ejection, you often have to get up to use the toilet at night);
- Quality of orgasm (still bright or blurred, pain in ejaculation).
The more details the patient remembers, the more complete the clinical picture that the doctor will prepare.
Differential Diagnostics
The symptoms of prostatitis are similar to those of many other diseases:
- Cystitis (cramps when urinating, lower abdominal pain).
- Adenoma (difficulty urinating, feeling of heaviness in the groin).
- Prostate cancer (blood in the urine, problems with urination).
- Pathologies of the rectum: hemorrhoids, paraplegia (inflammation), anal fissures, crepitus (ulcerative colitis)
Additional diagnostic methods and their rationale for use are shown in Table 1.
Table 1. Differential diagnosis of prostatitis
| Illness | Risk group | Analyzes |
|---|---|---|
| Hyperplasia | Men over 45 years of age with no history of urethritis, catheterization, bladder and urethral trauma (circumstances that may explain pain, blood in the urine)Prostate ultrasound and digital examination | |
| Prostatitis | Mostly young men who have recently had a fever, hypothermia, in the history of which there are no provocative factors (identical to hyperplasia) | ultrasound, whole blood count (CBC), digital prostate examination |
| Prostate Cancer | Men over 45, without a history of causing factors | Prostate ultrasound, PSA analysis, digital examination |
If necessary, other specialized doctors are involved in the diagnosis: proctologist, neurologist, vertebrate. The last two experts identify the causes of pain associated with a violation of the structure of the spine, a violation of the nerve endings.
Correct palpation
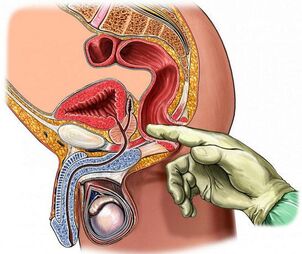
Digital rectal examination is the most affordable and informative method for checking the condition of the prostate. During the procedure, the doctor pays attention to the following parameters of his structure:
- Volume?
- Density?
- Surface roughness?
- Homogeneity (tissue homogeneity);
- Borders (contour clarity);
- Preservation of the isthmus (longitudinal suture between the lobes).
In prostatitis, the gland swells due to swelling (asymmetry is possible), its consequence is elastic, the longitudinal groove (suture) is not palpable and when touched, the patient may feel pain.
For a clear picture of this type of diagnosisrequirespreparation:
- Do not ejaculate the day before, do not drink alcohol, avoid strenuous exercise, hypothermia and overheating.
- Do not ride a bicycle for a day, do not use rowing machines (do not injure or massage the prostate this way).
- Before seeing a doctor, make an enema (a small enema can be used) to clean the rectal ampoule.
You can feel the prostate at a depth of 3-5 cm from the anus. The doctor performs the procedure with sterile gloves, lubricating the finger with gel. The patient is on his side with the knees hidden or standing in an elbow-knee position.
Laboratory Methods
Laboratory methods for diagnosing prostate inflammation include the study of biomaterials for the presence of pathogens.
Blood
Based on the results of general and biochemical blood tests (take capillaries from one finger), prostatitis may be suspected at an early stage. The analysis is done on an empty stomach in the morning. You should avoid smoking one hour before the procedure.
Important indicators:
- Leukocytes (blood cells, the number of which increases with a decrease in immunity in the context of inflammatory reactions). Normally from 4-9 × 10 ^ 9 units.
- ESR (erythrocyte sedimentation rate). The norm is about 5 units, an increase indicates inflammation or oncological process.
- Lymphocytes. Normally, the percentage of total blood cells ranges from 18 to 40 units. Excess means infection.
Men over the age of 40 are given the PSA test- a tumor index that exceeds a value that indicates chronic prostatitis or prostate cancer.Norm- less than 4ng / ml, after 50 years - 5, 53 ng / ml.
urine
The urethra passes through the prostate (the protective part of the urethra), so when the gland becomes inflamed, the urine changes color and consistency. To diagnose prostatitis, three types of tests are performed:
- General - determination of physical and chemical parameters. Signs of inflammation of the prostate: urine is cloudy, white, alkaline, there are proteins, leukocytes, purulent fibers, sometimes foam or blood. With massive prostatitis, phosphates are found.
- Cytological - examination for the presence of pathologically damaged cells. The presence of erythrocytes and epithelium may indicate a tumor process.
- Bacteriological - detection of traces of activity of pathogenic microorganisms. To do this, make a tank sowing residue in medium. If there are bacteria and fungi, then after a while they begin to multiply actively. Escherichia coli often causes prostatitis.
Before urinating, you should avoid eating salty and spicy foods, do not consume alcohol and coloring products (beets, coffee) The analysis is done in the morning on an empty stomach.For prostatitis, the three-glass test method is used:the patient urinates alternately in each glass. the result is the first, middle and final part. This method allows you to locate the inflammation: urethra, prostate, bladder. The four-eyed method is more informative. The last part of the urine is collected after prostate massage to obtain the secretion.
Secret prostate and sperm
Prostate juice is a valuable diagnostic material. Prepare for the fence in the same way as for a rectal digital examination. In order for the volume of the secretion to be sufficient, you should avoid sexual intercourse for three to five days.
Prostate secretion test methods:
- Microscopy?
- Backseeding;
- PCR (polymerase chain reaction).
PCR is the most accurate method. For the processing of the biomaterial, special enzymes are used that multiply the number of DNA fragments and RNA of the pathogens. Research requires a special device - an amplifier. More specifically, real-time PCR. The result is ready in an hour.
Inflammation of the prostate is indicated by the presence in the juice of amyloid bodies, staphylococci, streptococci, Pseudomonas aeruginosa, epithelial cells (more than three units per field of view). The number of fat cells decreases and the number of leukocytes increases.Thespermatogram for prostatitis is an additional analysis. In the context of inflammation of the prostate, the sperm becomes yellowish or brown, its viscosity increases (liquefies for a long time), there is pathogenic microflora. In chronic prostatitis, there are glandular epithelial cells, amyloid bodies and mucus.
Urethral swab
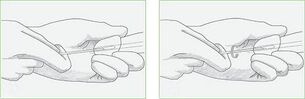
Urethral swab (scratch) is a less informative method for diagnosing prostatitis by secretion analysis.Used in cases where it is impossible to get the latter due to hemorrhoids, worsening of inflammation, the presence of calcifications in the body of the prostate.
The process for obtaining the material is quick but unpleasant: the doctor dips a brush into the urethra, which captures part of the cells that cover it along with microorganisms. The biomaterial is then examined by PCR, which allows you to determine the presence of pathogens in any quantity. The cause of prostatitis can be infections of the genitals: chlamydia, Trichomonas, mycoplasma.
Before the analysis for a day, you should refuse sexual intercourse in the morning, perform only external penile hygiene procedures (do not put anything in the urethra), do not urinate for two hours.
Organization methods
Organ diagnostic methods allow you to confirm and complete laboratory test results.
Ultrasound and TRUS
Ultrasound examination of the prostate makes it possible to visualize the structure, its contours, the nature of the tissues. In case of prostatitis, transverse ultrasound (TRUS) is considered the most informative: the doctor inserts the detector in the rectum. Prepare for the procedure in the same way as for palpation of the gland. An abdominal ultrasound (through the abdomen) is more comfortable for a man, but the prostate is not fully visible due to the bladder.
With inflammation of the prostate, its structure is heterogeneous, the contours are blurred, there may be foci of fibrosis (excessive connective tissue), scars. The prostate is enlarged, the groove between its lobes is smoothed.
MRI, PET and CT
If the ultrasound suggests the presence of a tumor process, your doctor may order a CT (computed tomography) or magnetic resonance imaging (MRI) scan to clarify the picture. The latter type of research is more accurate, but also more expensive. The procedures are painless, in terms of information content, they can replace a biopsy (bite from a tissue fragment).
CT and MRI show in detail the structure of the prostate: stones, cysts, tumors, inflammatory foci, structural abnormalities. For a clearer picture, a contrast agent is pre-injected into a vein (not used for men with kidney failure). For the procedure, an appropriate type of CT scan and rectal probe is used.PET - Positron Emission CT. It allows you to analyze the state of the prostate at the cellular and molecular level. It determines not only the presence and size of the tumor, but also the speed and quality of metabolic processes that occur in it.
Regarding preparation:the rectum must be emptied. Do not eat for five hours before the procedure.
Characteristics of the diagnosis of certain types of prostatitis
Acute bacterial (infectious) prostatitis is diagnosed based on patient complaints, urination, ultrasound, urethral smear. With active inflammation, the gland is painful, structural interventions are not allowed, in extreme cases, careful examination of the fingers.
Laboratory data for the diagnosis of acute prostatitis are not very informative. A urine culture may be appropriate, but it is not required. With active inflammation, there is no time to wait for results. Antibacterial treatment with broad-spectrum drugs is performed to relieve the symptoms.
Chronic prostatitis is practically not manifested in any way, therefore, its detection requires a whole range of laboratory, natural, instruments. Determination of the patient's immune and neurological status may be required.
Palpation of the gland, urine and prostatic secretions are of paramount importance. The presence of more than 10 leukocytes in the visual field indicates inflammation. If the bacterial culture does not allow the growth of infectious microflora in the context of an increased number of leukocytes, then an analysis for genital infections is necessary.
Due to the bacterial nature of inflammation in urine and prostate juice, there are a large number of pathogens. An indisputable microbiological sign of chronic inflammation: the number of germs (CFU) is greater than 104 per ml. Some of them number in the tens, so their presence in an amount of 10 to 102 per ml may indicate prostatitis.
Ultrasound does not always show chronic inflammation. In addition to the above methods, your doctor may prescribe uroflowmetry - a measurement of urine flow rate using special sensors.
Typical comorbidities
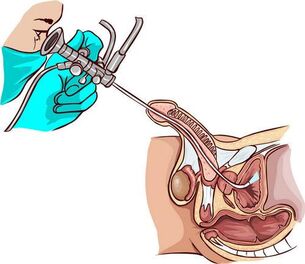
For long-term chronic prostatitis with signs of colitis (inflammation of the sperm near the prostate), urethroscopy is used- a visual canal examination using an endoscopic device. It helps to identify the narrowing of the urethra, violations of its structure, the condition of the orifices of the secretory ducts of the prostate (mucus, pus, thickening) and the tuberculous sperm.
Interpretation of results (determination of the stages of prostatitis from the condition of the sperm of tuberculosis):
- First: the tubercle of the seed is red, swollen, bleeding The same pattern is observed on the back of the urethra.
- Second: the periodic increase and decrease of redness and swelling is characteristic.
- Third: cystic changes occur in the tissues of tuberculosis and urethra, due to which the ureter lumen may narrow (narrow).
Ureteroscopy irritates the sperm duct receptors, which leads to reduced microcirculation and motility of the prostate, so the procedure is not performed unnecessarily.
Cystitis is also a companion of chronic prostatitis. Inflammation of the bladder wall is detected using ultrasound and cystoscopy. During the examination, pathological changes in the mucous membranes are identified, especially in the neck area. The condition of the bladder in the context of chronic prostatitis (sclerosis of the prostate):
- Cellular deformity of the bladder triangle. Enlarged ureter mouths.
- Narrowing of the neck.
Cystoscopy is prescribed in the final stage of the examination in the presence of lower abdominal pain and frequent urination.
The most difficult diagnosis is chronic bacterial prostatitis with pelvic pain of undetermined origin. In these patients, doctors first conduct research to rule out cystitis and neuropsychiatric pathologies.
How to diagnose prostatitis at home
A man may suspect acute prostatitis with the following signs:
- Severe pain in the lower abdomen and groin (between the testicles and anus).
- Increased body temperature.
- Pain when urinating (such as cystitis).
- Premature and painful ejaculation.
The same symptoms occur when chronic prostatitis worsens, caused by hypothermia or alcohol intake. The development of this form of pathology can be evidenced by the periodic appearance of blood in the urine, dull pain in the perineum (especially in a static position), difficulty urinating, worsening of the erection. Such points are the reason for communicating with a urologist.
Conclusion
The longer the inflammatory process in the prostate lasts, the more difficult the treatment will be, so you should not delay the diagnosis. In government services, most follow-up procedures and treatment are free.


























